DNI 7 Contribute to the production of dental images Workbook
INTRODUCTION: DNI 7 Contribute to the production of dental images Workbook
Click here to access top-notch assignment help provided by our native assignment help company.
This workbook accompanies the radiograph session delivered by your tutor will consist of a series of questions and require you to research information.
You will use varying methods to enable you to complete these questions. All can be completed using either written, typed, or audio answers to demonstrate your knowledge and understanding of how you support your service users within your setting. Discuss with your tutor and decide your preferred method.
This unit has three learning outcomes
The learner will:
- Be able to assist during the taking of dental images.
- Be able to process dental images.
- Be able to contribute to the quality assurance process of dental images.
Evidence requirements
Minimum requirement of one observation. Supporting evidence of learner understanding must be completed and provided in order to support performance evidence. Simulation is allowed for this unit.
Unit DNI 7: Contribute to the production of dental images (K/618/4914)
This unit focuses on the knowledge and skills required when assisting the operator throughout the dental imaging process.
Guided learning hours for unit DNI 7 is 16 hours.
This unit is mandatory and is not graded all criteria must be met before completion of this unit.
This unit will also have clinical observations by an assessor.
Relationship to GDC Learning Outcomes:
1.7.3, 1.8.1, 1.8.3, 1.11.1, 1.11.2, 1.11.4, 5.1, 8.1, 12.1
Relationship to Dental Standard Knowledge, Skills, and Behaviours
K27: Know and understand the scientific principles of medical ionizing radiation
K28: Know and understand the statutory regulations about radiography
K29: Know and understand the different types of radiographs used in dentistry including how to process and store them

Task1
(learning outcome 1, assessment criteria 1.1, 1.2,1.3, 1.4,1.5,1.6,1.7 and1.8)
1. What is the correct way to check that the imaging equipment is fully functioning and ready for use? How often should imaging equipment be checked?
|
A quality assurance program to change the images is necessary to ensure the standard of the images. The equipment must be monitored regularly to ensure the consistent operating facility of the images. The images produced by the equipment must be checked thoroughly to ensure the authenticity of the image and if that needs any changes then the changes must be done accordingly (Morid et al., 2021). “Darkroom safe lighting” is also checked for any leaks, and the digital sensors are verified once a year. Yearly calibration of the X-ray machines is also conducted. Test for the equipment for tightness of light and film screen should be checked half yearly or sooner in case of detection of any fault. |
2. What FOUR items could interfere with the radiographic image? How should individuals be asked to remove them?
|
Beam energy: The energy spectrum that is utilized in the formation of the image is directly proportional to the anode target's atomic number. The utilization of beam energy is necessary to analyze the amount of filtration produced for the image. Higher-intensity energy radiation gives rise to more scattered radiation. |
|
Acquisition geometry: It affects the quality of the image including the size of the spot and focal point along with the magnification amount. Geometric correction methods would be advisable in this case, including orthorectification and polynomial rectification. |
|
Magnification: An increase in the receptor distance between the patient and the image or an increase in the air gap leads to magnification enhancement. A fault in the image receptor can give rise to higher magnification. This phenomenon enhances the magnification amount and the produced image becomes blurry. |
|
Detector performance: A larger size of the detector element leads to low resolution, and this could be resolved by maintaining the size. It depends on the size of the element and can make a change in the resolution of the image. Individuals must be asked to control the interference of the above-said items. The interference of beam energy might be reduced by using a certain amount of energy that is exactly needed for the radiographic image. The focal point of the image must be adjusted as per the distance required to reduce the interference of acquisition geometry. The fault in the image receptor should be checked regularly to maintain the magnification range |
3. Radiography does not come without its risks. Explain what concerns individuals (adults, children and young people, older people, and those with additional needs) may have regarding dental imaging. If you could not allay their concerns, who would you refer the questions to?
|
Several research works have led to the conclusion that increased exposure to X-rays makes a patient more susceptible to brain cancer. The main concern of dental imaging implies the abnormality of the cells that leads to cancer. Such higher radiation can cause cancer in children and is assumed to create risk in the case of pregnant women. The questions regarding the concerns must be referred to a doctor to analyze the facts and take precautions to minimize the exposure of radiation to children and other patients. Also, patients having metal plates set in the dental structure are recommended to avoid X-ray imaging. This is because the anatomy that is to be diagnosed can be obstructed by the metal. Besides, the metal is likely to turn into any other active form in the presence of the rays. In case of failed attempts to answer the patients' concerns, they would be referred to senior professionals. |
Task2
(learning outcomes 2 and3,assessment criteria 2.1,2.2and2.3)
1. Describe the chemicals used in developing a radiograph and what they co
|
According to Galvao et al., 2019 The chemicals used in developing a radiograph include a developer and a fixer solution. Developer solution ● Developing agents: The combination of the chemicals helps to produce an image with different shades. It contains Hydroquinone (para-dihydroxybenzene), Elon (monomethyl-para-amino phenol sulfate), metal (l-phenyl-3-pyrazolidone)”. ● Preservatives: The preservative leads to the formation of sulphonate by preventing the oxidation process of the solution It contains Sodium sulfite. ● Activators: They provide an alkaline medium that is required by hydroquinone to react, and these are required to make penetration of the developing agent for the softening of the gelatin in the present emulsion). Sodium carbonate, sodium hydroxide, sodium metaborate, and sodium tetraborate are some of its constituents. ● Restrainer It helps to reduce the depression of the unexposed crystals and acts as an anti-fog agent., and it is made up of Potassium bromide. ● Hardeners: Glutaraldehyde is a type of hardener and It prevents the process of sticking and softening the emulsion. ● Fungicides: These prevent any kind of bacterial growth. ● Solvents: It contained distilled water. It can dissolve the chemicals to enhance the path of reactions. ● Buffers: These help in maintaining the developer’s pH. Fixer Solution: ● Fixing agent: It is made up of “Sodium thiosulphate (hypo)” or “ammonium thiosulphate”. It contains sodium and ammonium thiosulphate. it helps to remove all undeveloped silver crystals. ● Preservative: it contains sodium sulfite and prevents deterioration. ● Hardening agent: Potassium alum is used as a hardening agent. The main work of the preservative is to harden the emulsion of the gelatin. ● Acidifiers: They contain sulphuric acid and stop the further development of the developer. |
2. Explain what is wrong with the following radiographs and give them a quality assurance grade of 1,2 or 3.
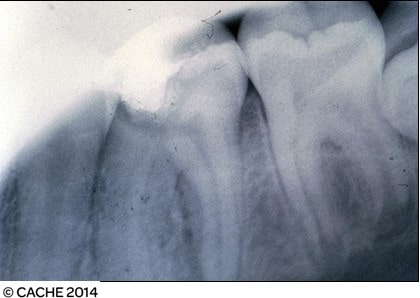
Fault: Blurry image
Grade: 2
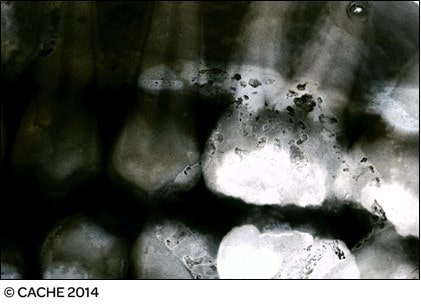
Fault: Black line, dot artifact
Grade: 2
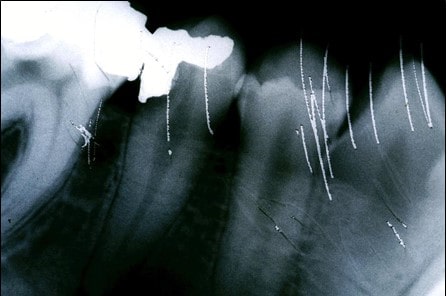
Fault: Apices are cut-off, blurry image, dot artifact, dropped film corner, black line, distortion
Grade: 3
Task3
(learning outcome 3, assessment criteria3.1 and3.2)
1. Explain the procedure at your surgery for producing dental I (NB: only one type of procedure should be given.)
|
The procedure for dental imaging in surgery is “Long Cone Periapical Radiography”, which captures the image of one or two teeth. The procedure of the surgery is Long cone periapical radiography and it helps to capture the image of the condition of one or more teeth (Reinhart et al., 2020). the procedure involves the following steps: 1. The identification data of the patient is checked, followed by the preparation of the patient. It analyses the condition of a patient to make any changes in the denture. 2. The image receptor is inserted into the film holder to ensure that it is aligned with the X-ray beam. The film holder is then inserted into the mouth of the patient keeping it parallel to the palatal aspect of the tooth (Marc El Hage et al. 2019). The process ensures the alignment of the beam and holds the film to capture consistent images 3. The patient is then asked to close the mouth onto the bite block, which is supported by a roll of cotton wool. This ensures that the gaps between the teeth are filled and provides support to the block. The next process includes the filling of the gap between teeth and the position of the X-ray cone to develop uninterrupted images. 4. It includes the removal of the exposure factors. It helps in the processing of the image receptor. 5. The image is assessed for the final quality in the last stage of the process to ensure that it has the correct density. It ensures the correct density and contrast of the viewable and differentiated parts of the teeth. The image is reported in the clinical notes for complying with the “IRMER – Ionising Radiation (Medical Exposure) Regulations” in the UK. |
2. How do you ensure that the quality of the image is maintained throughout the procedure?
|
The criteria that are followed in the process to ensure the image quality include: ● Constant checking of the image receptor for preventing displacement in the mouth. ● Placing of image receptor adjacently with the object. ● X-ray cone should be attached parallelly to reduce radiation. ● The front edge of the X-ray cone is to be kept parallel to the receptor to prevent cone cuts and images that are obliquely positioned. ● the exposure voltage should be maintained to get rid of any kind of chaos. ● Contamination through saliva has to be prevented, for which the barrier wraps are disposed of after removing the film holder. ● Quality assurance of the image is conducted to ensure the authenticity of the receptor while obtaining the produced image. |
3. What is your surgery procedure for storage of images?
|
The final images must be stored digitally to get access anytime from any device. The storage of the images relies on the format used by the respective authority for future uses (ncbi.nlm.nih.gov, 2022). A prototypical “HIPAA-compliant Medical Imaging Management System” would be used to request access to the PACS. The intermediary system would be an Edge-server which would play the role of a requesting node such that other physicians can also have access to the images. |
Learnerdeclarationofauthenticity: DNI7
I declare that the work presented for this unit/task is entirely my work.
Learner signature: Date:
For an e-portfolio, a signature is not required, provided the learner has a personalized and secure login.
REFLECTIVE ACCOUNT
Think about what you have learned during this unit. How has your knowledge improved and how have you applied this to your working practice? Please reflect below on the workbook you have completed by answering the following questions.
What have you learned or how has this reinforced what you already knew?
|
The risks associated with dental imaging were already known to me, but most of it was based on preconceived notions. Although most of the beliefs I have regarding the risks are partially true, I have got to learn more facts about the process from the existing literature while doing this assignment which I had a rare idea about. The compounds that are used to produce the image were known to me, but I have gained an insight into their actual functions. I have developed a critical thinking ability through the identification of radiographs which I usually perform daily. Also, I have got to learn about the detailed process of "Long Cone Periapical Radiography”, along with the justification of each step. Being in the clinical profession, the storage procedure of a radiograph is known to me, but I got to learn about the software and hardware involved in the storage process in the course of this assignment. |
What was good about completing this workbook?
|
Most of the duty hours of a clinician are spent resolving an error occurring in any surgical process. We rarely get time to analyze the factors that have contributed to a particular error in radiographic imaging. I have to learn about the potential factors that might hamper the imaging process or deteriorate image quality. Hence, now I know about the preparations that I would need to take beforehand to ensure that the images captured are of good quality. The radiographs provided in the workbook enabled me to practice error identification which I am obliged to perform daily during my duty hours. The detailed process of “Long Cone Periapical Radiography” is now known to me, but I might have to assist in the future. |
What did you find difficult?
|
The thing which I found difficult is the surgical process of “Long Cone Periapical Radiography”. Although I read about the justification while doing this workbook, the entire process has been overwhelming. The process involves too many steps, and any minor error might lead to a faulty image. The storage process of the images is also too complicated for a clinician who has limited knowledge of technology. On the other hand, this information is necessary to ensure that I am storing the images properly and allowing access to other physicians. |
How will your learning be used in practice?
|
I can use the knowledge gained in this assignment for future surgical procedures I conduct in the future. I have developed a thinking ability which I suppose might be helpful in the future. The criterion required to ensure image quality would help me in the future while I assist doctors in the surgical process. The practice gained in the identification of radiograph errors has provided me with the ability to identify quicker, which I consider would help me further. |
|
How long has it taken you to complete this workbook? |
6 |
HRS |
15 |
MINS |
References
Anastasio, A., 2021. Dental radiography–and you. Dental Nursing, 17(2), pp.72-76.
Cleveland. 2021. Oral Surgery.
Galvão, N.S., Nascimento, E.H.L., Lima, C.A.S., Freitas, D.Q., Haiter-Neto, F. and Oliveira, M.L., 2019. Can a high-density dental material affect the automatic exposure compensation of digital radiographic images?. Dentomaxillofacial Radiology, 48(3), p.20180331.
Laneve, E., Raddato, B., Dioguardi, M., Di Gioia, G., Troiano, G. and Lo Muzio, L., 2019. Sterilization in dentistry: a review of the literature. International journal of dentistry, 2019.
Marc El Hage, D.M.D., Nurdin, N., Abi Najm, P.S., Bischof, M.M. and Nedir, R., 2019. Osteotome sinus floor elevation without grafting: a 10-year study of cone beam computerized tomography vs periapical radiography. Periodontics, 39, pp.e89-e97.
Morid, M.A., Borjali, A. and Del Fiol, G., 2021. A scoping review of transfer learning research on medical image analysis using ImageNet. Computers in biology and medicine, 128, p.104115.
ncbi.nlm.nih.gov , 2022 X-Ray Image Quality Assurance Available at: https://www.ncbi.nlm.nih.gov/books/NBK564362/ [accessed on: 31-10-2022]
Reinhart, G., Grange, D., Abou-Khalil, L., Mangelinck-Noël, N., Niane, N.T., Maguin, V., Guillemot, G., Gandin, C.A. and Nguyen-Thi, H., 2020. Impact of solute flow during directional solidification of a Ni-based alloy: In-situ and real-time X-radiography. Acta Materialia, 194, pp.68-79.
Shashikala, J. and Thangadurai, N., 2021. Evaluating spatial and frequency domain enhancement techniques on dental images to assist dental implant therapy. International Journal of Electrical and Computer Engineering, 11(6), p.5019.



